Medicine has always been a hard taskmaster, yet more and more we hear about the unrest and dissatisfaction of doctors across the world
“Devalued, demoralised, and depressed” read the placard held high above the heads of junior doctors during their 2016 NHS strike. These three words perhaps best sum up the prevailing mood of many doctors, not just in the NHS but across the world. We continually hear about the growing malaise among medics—a phenomenon that is often reported as self-evident. The question is are doctors objectively unhappier than in previous years, and if so, why?
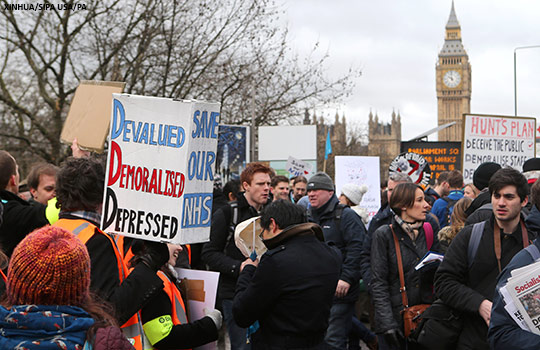
Unfortunately, there are only a few well conducted, longitudinal studies that use the same methodology and diagnostic instruments to help answer this question. There is also the problem that most studies measure variations of burnout, dissatisfaction, and stress, all of which are difficult to define and even if present do not always translate into formal mental illness, such as depression or anxiety. It’s worth examining what evidence there is though, lest we risk being caught up in the tide of a worldwide self-fulfilling prophecy built by contagion and case finding.
So, looking briefly at the evidence. A study of American doctors using the same methodology examined satisfaction in 1986 and again in 1997. Overall, physicians in 1997 were less satisfied in every aspect of their professional life than 1986 physicians. Differences were significant in three areas: time spent with individual patients, autonomy, and leisure time. The Kaiser Family Foundation have conducted postal surveys of doctors’ opinions based on representative random samples in 1981, 1999, and 2001. Doctors reported that their and their colleagues’ morale had gone down in recent years and nearly half would not recommend the profession today. Administrative hassles and loss of autonomy are cited as the main reasons for dissatisfaction, followed by excessive professional demands, less respect for the medical profession, and inadequate financial rewards. Other studies cited in an American review also show greater dissatisfaction and a worsening of wellbeing in more recently qualified doctors compared to older doctors.
In England, researchers have surveyed general practitioners eight times, using the same methodology between 1998 and 2015. The 2015 study showed the lowest levels of job satisfaction and highest levels of stress since the start of the survey series, as well as an increase in the proportion of GPs intending to quit direct patient care within the next five years. The UK charity the Royal Medical Benevolent Fund conducted a postal survey of almost 2000 senior doctors in 2017. Ninety two per cent said that working conditions in UK hospitals had deteriorated in the past decade.
There are other studies, however, which do not show this deterioration. Jenny Firth-Cozens carried out a longitudinal study on doctors’ wellbeing and views of their job, starting in 1983. Over the years she found that some areas stayed the same, some got worse, and some got better. The level of stress remained remarkably constant at around 28%. What did change over the years was that doctors were more able to disclose stress and discuss their problems with their peers. A systematic review of satisfaction among American doctors found 97 articles published between 1970 through to 2007. Overall, physician satisfaction remained relatively stable, with small decreases found only among primary care physicians. There were similar findings in a study of the stress and wellbeing of Australian junior doctors compared with those in America and the general population conducted at points between 2009 and 2014. Junior doctors in 2014 reported better overall mental health, more satisfaction with their clinical posting, and were less stressed compared to those in 2009, though they were significantly more stressed than the general population.
Overall these studies do little to give a clear impression of whether dissatisfaction has increased; whether we are measuring doctors’ wellbeing more stringently; or whether doctors, as Firth-Cozens surmised, are now more able to disclose distress than previous generations might have been. There seems to be some validity to this latter theory, as past generations of doctors tend to talk with such nostalgia about their time in training or as junior doctors that it is hard to imagine any of them were struggling to cope with the pressure and intensity of their work. An informative piece in The BMJ interviewed doctors who worked in different decades from the 1940s to the present day. The doctors who trained before 2000 recall fondly their team working, their “firm,” and the camaraderie of the doctors’ mess. They broadly seem to agree that, however tired they were, it was better to be a trainee doctor in the past than it is now.
If doctors are unhappier today than in yesteryear, why might this be? So many factors have changed in how doctors are chosen, trained, work, remunerated, monitored, and inspected over the past decades that trying to unravel what might be causative is difficult. Factor in changes in the complexity of medical care, patient autonomy and expectation, and wider sociopolitical and financial changes and it becomes even more difficult to find a single explanation. For example, an obvious change in recent years is the gender profile of doctors, with women now making up the majority of entrants to medical school. While gender might play a part, untangling the contributing factors (including the multiple roles women have beyond the workplace and that women may be more willing to disclose mental illness and attend treatment services) is difficult.
Another area of great change has been how students and doctors are trained—with packed curricula and more focus on continuous assessment as well as final examinations. Tellingly, when one American medical school introduced changes to their training programme, which resulted in students spending less time in class or studying each day compared to other US medical students, these students reported lower stress, less exhaustion, and a greater sense of engagement in medical school. They also had improved quality of life, mental health, and academic performance.
In the NHS, training rotations are now far more geographically diverse than in previous generations. Doctors move rapidly from institution to institution, operating more like itinerant workers than resident doctors as a result. These factors undermine the ability to build cohesion among doctors or continuity of care for patients. Yet it is exactly this kind of continuity—in terms of looking after patients from admission to discharge, as well as continuity of space (in wards, hospitals, and homes) and colleagues (peers, trainers, and nursing colleagues)—that is so important for the wellbeing of doctors and patients alike.
Healthcare environments have always been emotional places to work in and medicine is a hard taskmaster. What has changed is therefore not what goes on within the hospital, but rather how care is delivered and how staff are treated. Doctors now complain of having little control over their working hours, space, days off, job security, authority, and no guarantee of support from superiors when things go wrong. The growing culture of litigation and media scrutiny leaves little room for error and increasingly calls for doctors to be named, blamed, and shamed.
Doctors are caught in the crossfire of the changing positions of individuals in society and especially the redistribution of power and authority. Furthermore, the industrialisation of medicine, with its focus on productivity and profit, conflicts with the values of medicine and causes widespread anxiety. It impacts especially doctors’ professional self-identity, changing the role of medicine from “a craft concerned with the uniqueness of each encounter with an ill person, to a mass manufacturing industry preoccupied with the throughput of the sick.”
The majority of doctors still take satisfaction in their work, are not mentally unwell, and thrive in their job. Focusing on the ill health of the few may risk contagion of the many and put people off a profession, which over the course of a career is sustaining, well paid, and secure. The evidence of increasing unrest and dissatisfaction among doctors, however, cannot simply be ignored or dismissed as inconvenient. While many root causes are intangible, amorphous, and borne out in different studies to varying extents, it is undeniable that the position of the doctor within society has altered dramatically and it is most likely that it is this change that is causing such distress among the current generation of doctors.
 Clare Gerada is the medical director of the Practitioner Health Programme and GP Health Service. She will be chairing the first day of the International Practitioner Health Summit 2018: The Wounded Healer, 4-5 October 2018.
Clare Gerada is the medical director of the Practitioner Health Programme and GP Health Service. She will be chairing the first day of the International Practitioner Health Summit 2018: The Wounded Healer, 4-5 October 2018.
Competing interests: Nothing further to declare.
