By John Orchard (@DrJohnOrchard)
The Scandinavians have done it again – leading the world of orthopaedic outcome research with the first high-quality RCT to assess Total Knee Replacement (TKR) [1]. Danish investigators randomised 100 eligible patients (average age 67, BMI 32) to either TKR (n=50) or conservative care (n=50). Fortunately for knee surgeons – who have copped an absolute pounding from Evidence-Based Medicine in recent years regarding use of knee arthroscopy in knee osteoarthritis [2]– the headline read “TKR effective at significantly decreasing pain and increasing function”. Also, 26% of those randomised to non-surgical treatment crossed over to TKR during the 12 month follow-up period. The non-surgical group also improved over the 12 months, and the authors couldn’t rule out an additional surgical placebo effect contributing to the improvement over and above the trial effect for the non-surgical patients.
The sting in the tail for the surgical results was that the TKR group had a much higher rate of related (which was expected) and also general medical (less expected) complications over the 12 month follow-up period. Serious complications thought to be related to the surgery or knee OA occurred in 16% in the surgical group versus 2% in the non-surgical group. However, total serious adverse medical events in general in the populations were 48% versus 12% over the 12 month period. That is, having a TKR seriously challenges the patient’s general health in this older, generally overweight population. Not so much as, having a femoral neck fracture (e.g. there were no deaths in the TKR RCT, whereas femoral neck fractures among 80-year old women have an 8% first year mortality rate) but enough to warrant warning patients about this increased risk prior to their undergoing TKR.
This makes the decision as to whether to undergo TKR a very difficult one (and hence one that should be probably made by the informed patient rather than the surgeon): do the more likely improvements in pain and function of a TKR outweigh the significantly increased risk of a serious adverse event if I decide on surgery?
In helping to advise a patient on this difficult decision, here are factors to take into account:
TAKE THE FOLLOWING INTO ACCOUNT
(1) Current fitness level. Pain is subjective but fitness and activity levels are objective. No one likes pain but if the pain is bearable you can safely live with some. Low activity levels are very hazardous to long term health – we now know it is dangerous to be immobile/sedentary.
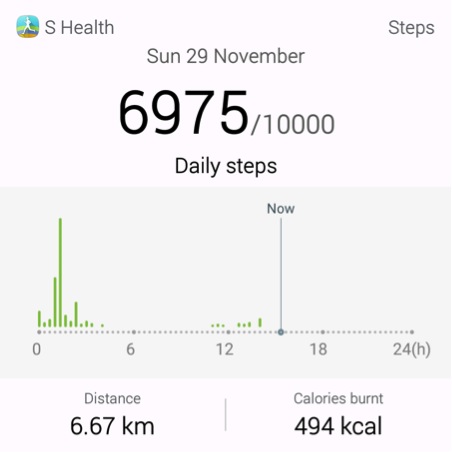
Thus, if knee pain is preventing a patient from being able to undertake adequate regular exercise, then the benefit of TKR is substantially increased, as the procedure offers the potential to exit this high risk group. We can quantify adequate physical activity easily with respect to walking – about 6000 or 7000 steps a day is adequate – and if the knee allows this level of activity the imperative for TKR should be a lot less. Steps per day can easily be measured using a fitness tracker or smartphones (Figure 1).
(2) Background medical risk. Given the main argument against TKR is the risk of major medical complication, a person with higher than normal baseline medical risk should be more cautioned against surgery. Pre-existing cardiac or renal disease, history of DVT requiring anti-coagulation, being a smoker, and diabetes are all relative contra-indications, as they increase the risk of catastrophic medical complication. If none of these risk factors are present, a patient may be in a lower risk group and can be more confident of avoiding serious complication.
(3) Recent cortisone injection into the knee [3] and previous knee arthroscopy [4, 5] (which both are erroneously still used routinely) lead to increased risk of complication in TKR. A patient who has had these interventions, especially recently, is in a higher risk group of a bad result with TKR and can be relatively advised to hold off.
(4) Whether conservative care has “failed” or simply has not been attempted. Unfortunately the success rate of conservative treatment of knee OA is not particularly encouraging, but success rates of certain treatments are not zero. Exercise programs (moderate loading) are recommended based on evidence, as is weight loss. Physiotherapy may help, particularly in cases where significant pain is arising from the patellofemoral joint (clue to this may be severe pain on steps or lunge movements). There is some evidence that hyaluronan gel injections or platelet rich plasma (PRP) injections can help in knee OA, and, in contrast to knee arthroscopy or cortisone injections, current evidence suggests that these can be attempted without penalty. That is, they provide a slightly better response than placebo injection, without major risk of significant harm.
HOWEVER DO NOT MAKE THE TKR DECISION ENTIRELY BASED ON THE FOLLOWING:
(1) X-ray or MRI severity of disease. The X-ray (MRI should generally not be used for a knee with OA) findings should establish the diagnosis of knee osteoarthritis, but there are some cases of mild-moderate OA on X-ray which have severe symptoms and other cases where severe changes on an X-ray are associated with mild symptoms only. “Treat the patient not the X-ray” applies here. Similarly it is speculative and probably an error for an expert to look at a knee X-ray and say “this knee has 5 years left in it – that’s when you’ll need to come back for a knee replacement”. Since function and X-ray severity correlate quite poorly, using X-ray to predict clinical deterioration is unwise. Walking tolerance is much more relevant to the TKR decision than X-ray severity.
(2) The patient’s age. There has been a tendency for some surgeons to proclaim “60-65 is the best age group to get a knee replacement, as patients are young enough to do well and old enough to potentially survive the rest of their life without needing a revision”. There is some truth in this logic, but it shouldn’t be used to encourage a patient of 60-65 years to undertake TKR when it is not really needed, as there is no automatic guarantee of deterioration. Similarly if a patient in 50s or even 40s is horribly debilitated by knee pain and unable to walk more than a few thousand steps per day, it could still be the correct decision to proceed with an uncemented TKR earlier in life on the understanding that a revision procedure will likely be needed.
*******************
John Orchard is an Australian sports physician. He has no conflicts to declare other than treating knee osteoarthritis patients in clinic, occasionally with injection therapies. His views are personal and not necessarily representative of organisations he is affiliated with. You can read more at www.johnorchard.com and/or follow @DrJohnOrchard on Twitter He is a Felllow of the Australasian College of Sports Physicians (ACSP) and the ACSP is one of BJSM’s 23 member societies.
References
- Skou ST, Roos EM, Laursen MB et al. A Randomized, Controlled Trial of Total Knee Replacement. N Engl J Med 2015; 373:1597-1606
- Thorlund J, Juhl C, Roos E, et al. Arthroscopic surgery for degenerative knee: systematic review and meta-analysis of benefits and harms. BMJ. 2015;350:h2747.
- Cancienne JM, Werner BC, Luetkemeyer LM, et al. Does Timing of Previous Intra-Articular Steroid Injection Affect the Post-Operative Rate of Infection in Total Knee Arthroplasty? J Arthroplasty. 2015 Nov;30(11):1879-82.
- Brophy RH, Gray BL, Nunley RM, Barrack RL, Clohisy JC: Total knee arthroplasty after previous knee surgery: expected interval and the effect on patient age. J Bone Joint Surg Am 2014;96:801-5
- Piedade S, Pinaroli A, Servien E, et al. TKA outcomes after prior bone and soft tissue knee surgery. Knee Surg Sports Traumatol Arthrosc 2013;21:2737–43.